
Leadless pacemakers are compact, wire-free devices that regulate heartbeats without invasive surgery. Chemical pacemaker batteries typically last about 10 years, but City Labs’ NanoTritium™ betavoltaic batteries offer a game-changing solution. With a lifespan of 20+ years, these nuclear batteries are small, safe, and require fewer replacement surgeries, improving patient safety and convenience.
Imagine if your phone needed surgery each time the battery died, that wouldn’t be very convenient. Especially if its battery life was only as long as it is right now.
When a battery-powered device is used to assist a human with essential bodily functions, it may need to be replaced one or more times. Those replacements typically do involve surgeries, and dangerous ones at that. That’s why scientists are working to make safe batteries for devices like pacemakers that will last as long as possible.
What Is a Pacemaker?
A cardiac pacemaker is a small device used to stimulate and measure the performance of someone’s heart. Hundreds of thousands of pacemaker implants are performed each year to tackle issues like bradycardia (a slow heartbeat). When someone has bradycardia, their heart may be unable to transfer sufficient blood throughout their body. A pacemaker can help speed up the heartbeat in times of need to keep the blood flowing properly.
How Does a Pacemaker Work?
A pacemaker typically consists of a small computer that is implanted into the soft tissue of your chest and connected to wires that connect directly to your heart. This computer relies on a battery to supply the power that it needs. The pacemaker monitors your heartbeat and sends impulses to pace your heart when it starts beating too slowly.
Additionally, the pacemaker tracks your heartbeat and stores the data. That way your doctor can evaluate the situation and, if necessary, adjust your pacemaker settings.
Leadless Pacemakers
A leadless pacemaker is different from a permanent pacemaker because it is implanted as its own individual device and does not get wired into the heart. Leadless pacemakers are a fraction of the size of normal pacemakers and are typically only used in patients who require single chamber electrical stimulation.
There are currently two types of leadless pacemaker batteries: lithium carbon monofluoride and lithium polycarbon fluoride. Both rely on an electrochemical reaction and begin to run out of power after around 10 years of use.
Implanting a Leadless Pacemaker
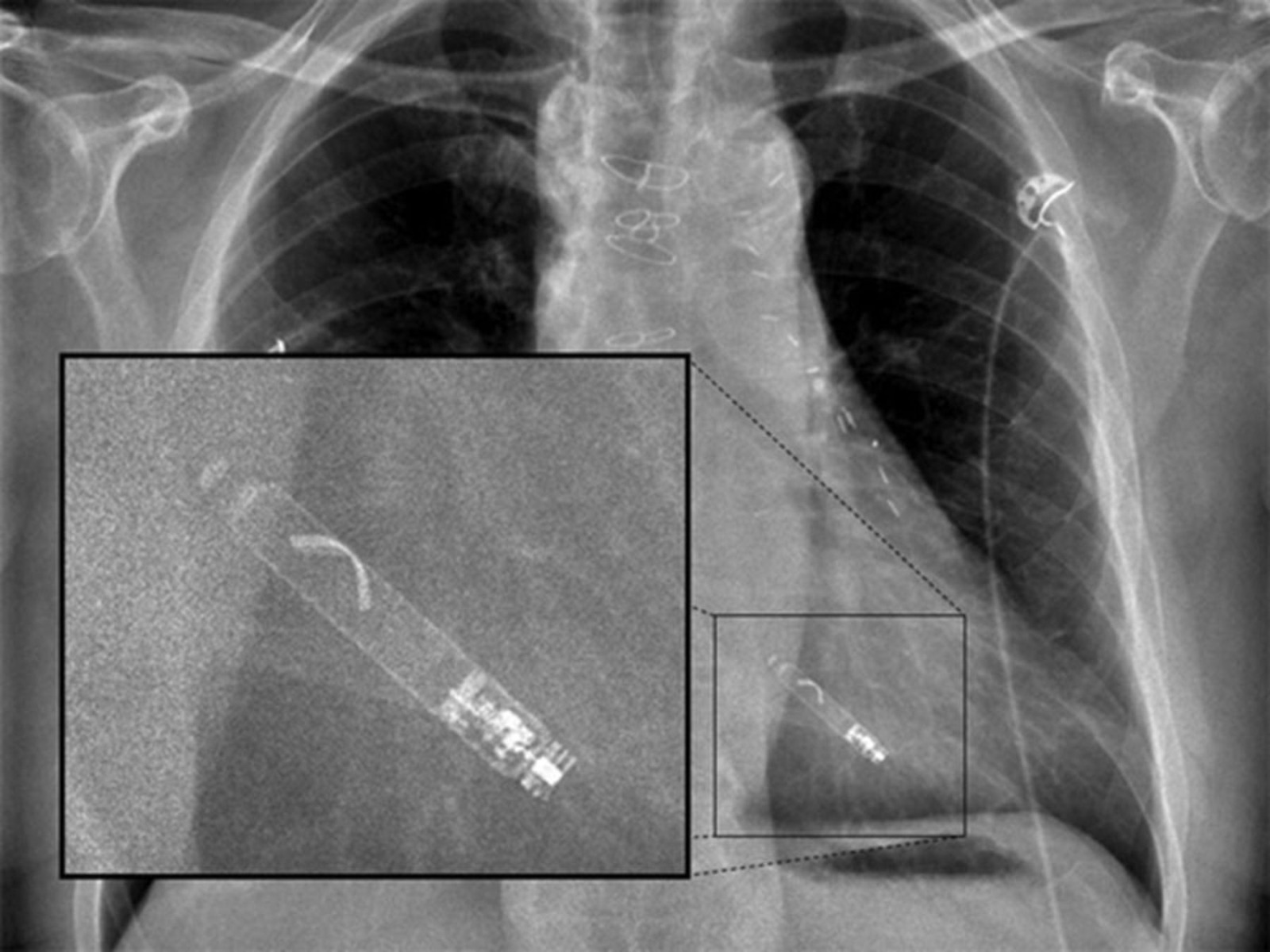
The process of implanting a leadless pacemaker is less invasive than that of a normal pacemaker. A doctor inserts a catheter into the femoral vein near your groin area and uses an X-ray device to guide the pacemaker to your heart. Once the device is properly placed, the computer can successfully monitor your heart and send electrical impulses to manage your bradycardia.
This procedure poses a much lower risk to the patient’s heart and does not leave any external scars or bumps on the chest.
What Is a Pacemaker Battery?
When a tiny computer is inserted into the tissue of your chest below the skin, there is no way to plug it in or recharge it. The only way to power a device like this is with a small battery that doesn’t damage its surroundings. As important as a pacemaker is, it’s absolutely nothing without a functional pacemaker battery.
Once implanted, pacemakers are difficult to access; the less a doctor has to perform surgery to put in a new battery, the better. For this reason, pacemaker batteries are low-energy power sources capable of lasting for extended periods of time.
How Long Do Pacemaker Batteries Last?
Most current pacemaker batteries only last 5-10 years before needing to be replaced. Pacemaker battery life depends on several factors—the most important of which is the power source.
While there is ongoing research to improve the lifespan of electrochemical pacemaker batteries, another type of battery already exists that can provide energy for a longer period of time: nuclear batteries.
Nuclear batteries were briefly used in pacemakers in the 1970s, but were ultimately discontinued because they were inconvenient and patients worried about hazardous side effects.
Nowadays, there are nuclear batteries available that have a lifespan of 20+ years with virtually no risk to humans. This evolution could revolutionize the pacemaker battery industry and help publicize the safe and effective use of nuclear batteries.
Pacemaker Battery Voltage
When selecting a cardiac pacemaker battery, it’s important to consider the minimum and maximum voltage of that power supply. The pacemaker should be capable of outputting an impulse somewhere between .1 and 15 volts up to 300 times per minute.
While the use is rarely this high or low, the exact impulses will depend on the specific patient’s heart. It’s good to prepare for the most extreme situations. It should be noted, however, that the more often a traditional leadless pacemaker needs to send electrical impulses, the sooner its battery will need to be replaced. With betavoltaic power sources, the battery’s output will not change based on how much it is used.
Pacemaker Battery Size
Traditional pacemaker batteries typically take up almost half the volume of the entire pacemaker device. They commonly weigh less than 30 grams and are circular or semi-circular. They conform to the shape of the pacemaker, which is manufactured without sharp edges to protect the surrounding tissue.
Betacel nuclear batteries—the first nuclear pacemaker batteries–were roughly 16 cm3, which made them less convenient. New nuclear pacemaker batteries are smaller and more streamlined, much like lithium batteries.
Leadless pacemaker batteries must be even smaller because they must be inserted into the ventricle of the heart.
Rechargeable Pacemaker Batteries
When implantable pacemakers were first created, they contained nickel-cadmium batteries that could be recharged. This required wireless recharging through the skin for multiple hours every few days.
Even while being recharged, the pacemaker batteries still had to be replaced frequently due to their short lifespan. When you are using a device to keep someone alive, you don’t want their survival based on whether or not they remember to charge it. This potential for patient error also contributed to the move away from rechargeable batteries and toward longer-lasting ones.
Trends in Cardiac Pacemaker Batteries
Over the years, scientists have tried many different strategies for developing pacemaker batteries. From rechargeable nickel-cadmium, to mercury-zinc, to lithium-iodide, pacemakers have seen much improvement.
That being said, this technology is nowhere near as good as it could be. City Labs is working to improve pacemaker batteries with the use of tritium as a power source.
Lithium Pacemaker Batteries
The most popular form of electrochemical pacemaker battery, first used in 1975, is the lithium iodine battery. Known to last 5-10 years, these batteries have two attractive qualities that set them ahead of the competition.
First, lithium pacemaker batteries have a low self-discharge rate, which increases their shelf-life. They do not expend much energy when they are not being used.
Second, they are very predictable. The stable voltage of a lithium battery remains constant for most of its useful life, then slows down gradually, making it very easy to plan replacements.
Nuclear Pacemaker Batteries
Nuclear batteries were used briefly in the past with the isotope plutonium-238 and Promethium-147. 238Pu has a half-life of 87 years, allowing it to maintain a sufficient current for multiple decades. However, because of their large size and the public’s concern about their potential toxicity, these early radioisotope thermoelectric generators were overshadowed by the introduction of lithium batteries. The 147Pm betavoltaic batteries were also too large to compete with newer devices.
As technology continues to develop, scientists are moving back toward nuclear batteries through the use of more controlled isotopes. Tritium, for example, is a relatively benign isotope of hydrogen with a half-life of 12.3 years. This means a tritium battery is capable of safely supplying a pacemaker with energy for more than 20 years.
Pacemaker Battery Replacement: How Often Do Pacemaker Batteries Need to Be Replaced?
A pacemaker is not the only implantable device that can go into the human body. There are plenty of other medical devices which regulate bodily systems and necessary processes. Since many of these devices are often powered by batteries, those batteries will eventually need to be replaced. However, implantable device replacement procedures require replacing the whole device.
In the case of a pacemaker, it must be hermetically sealed to prevent any liquid from interfering with the electronics. This means the battery is permanently embedded in the device.
As previously mentioned, the replacement procedure really only needs to take place when the power source runs out. If the power supply is not replaced, the pacemaker will not send any electrical impulses to stabilize your heartbeat, which can lead to dangerous side effects.
Assuming your pacemaker and pacemaker battery function properly, you’re looking at around 5-10 years with a current lithium-iodide power supply, and 5-10 years with a leadless pacemaker. The length of time a lithium-iodide pacemaker battery will last depends on the number of impulses it is required to send. Tritium battery power output doesn’t depend on how often it delivers life-saving stimulation. City Labs is looking to double the length of time a leadless pacemaker can operate before replacement becomes necessary.
While current competitors like Medtronic’s Micra and Boston Scientific’s Nanostim products last for roughly a decade, City Labs is working with Biotronik to develop the next generation of leadless pacemakers that will not need to be replaced for at least 20 years. These tritium betavoltaic batteries will be small, safe, and efficient.
Pacemaker Battery Replacement Procedure
To replace a permanent pacemaker battery, a doctor must remove the entire pacemaker and put in a new one. They will do this by making a small incision in the skin with local anesthetic (with or without light sedation). The doctor does not need to replace the wires in the patient’s heart, which makes it safer and less invasive than the original implant procedure.
Leadless pacemakers are typically not removed at all—if you need a new one, your doctor will just put it in next to the old one without risking a removal procedure.
Typically, the patient will remain awake throughout the surgery, and the whole thing will only take a couple of hours. Once the surgery is done, the patient should pay close attention to their medical team’s instructions to make sure there are no complications.
Pacemaker Battery Replacement Recovery
The recovery time for leadless pacemaker surgery is quick—patients are often allowed to leave the hospital on the same day as the procedure. Older patients may sometimes be asked to stay longer so their incisions can be monitored and cared for.
As with many surgeries, the doctor will recommend that you avoid heavy lifting and strenuous activities for a little while to prevent any sutures from coming apart. Within a few weeks, your recovery process should be complete and you can resume your usual routine with a new, fully-charged pacemaker.
When getting a new leadless pacemaker, the patient is required to lay straight with a flat leg for two to six hours after the procedure. This helps to prevent excess bleeding from the entry site. Aside from the typical risks of an incision, the leadless pacemaker replacement procedure poses a low risk to the patient. As mentioned earlier, it is unlikely that the patient will have a leadless pacemaker removed.
Pacemaker Battery Replacement Risks
Pacemaker battery replacement is viewed as a minor surgery with a high success rate, but that does not mean it comes without risks. It’s always important to talk to your doctor about the associated risks of any medical procedure so you know what you’re getting yourself into.
Traditional pacemaker battery replacement procedures can sometimes result in the following issues:
- Internal bleeding
- Blood clot formation
- Stroke
- Heart attack
- Infection at surgery site
- Damage to surrounding tissue
- New pacemaker malfunction
Minimizing these risks is an important part of why City Labs believes its pacemaker battery technology will benefit both patients and the medical community. Reducing the overall number of pacemaker replacement surgeries would reduce the number of surgeries that result in negative health consequences.
Limitations on Pacemaker Batteries
Optimizing this technology involves addressing all of the different hurdles at once. There are still many factors limiting pacemaker batteries, including:
- Size: Pacemaker batteries must be small enough to fit into the pacemakers themselves—which must be small enough to not inconvenience the host.
- Safety: The power supply must not pose a risk to humans; even if their duration is a bit longer, there is no reason people would risk radiation poisoning to put off surgery for one or two years.
- Power: Safe materials in a small concentration are rarely capable of putting out substantial amounts of energy.
- Lifespan: How long can the batteries go without needing to be replaced? Do they stop outputting energy at a certain point?
- Predictability: Will the doctor or patient know when the pacemaker battery is running low?
Replacement: The easier a pacemaker battery is to acquire and replace, the more individuals will opt for said product.
Most current and past pacemaker batteries have only been able to address a few of these at a time. For example, the plutonium nuclear batteries lasted a long time, but were too big and potentially toxic to humans. Lithium batteries are small, safe, and predictable, but don’t output the same power as other batteries and only last around 10 years.
City Labs has been working to develop a leadless pacemaker battery with its NanoTritium™ technology, which should soon be making its debut on the commercial market.
City Labs’ Betavoltaic Battery Products Supply Power for 20+ Years
Our products can provide long-lasting, low-energy power for more than 20 years by harnessing the radioactive decay of tritium. Unlike other isotopes, tritium relies on beta particles instead of alpha or gamma.
Beta particles are much easier to control and still provide power sufficient for small devices, including leadless pacemakers. See what else this technology has been used for in our historical review of betavoltaic batteries.
Understanding how betavoltaic sources work—and their potential applications—opens up a world of possibilities for nuclear battery technology.
Developing Research on Efficient and Affordable Pacemaker Batteries
City Labs’ NanoTritium™ batteries are already being used for a variety of different devices as affordable, long-lasting power sources. As a next step, we believe that the leadless pacemaker industry stands to benefit greatly from our technology.
We are looking to double the length of time a leadless pacemaker can last without needing to be replaced. The City Labs’ team also worked with Dr. Larry Olsen from 2009 to 2017, who was a part of constructing the first Betacel nuclear pacemaker batteries.
Reach Out to Discuss Our NanoTritium™ Batteries for Your Pacemaker Technology
If you are interested in learning more about City Labs, Inc., don’t be afraid to reach out to our team. We are happy to discuss the exciting applications, benefits, and opportunities that this technology offers.
We are looking for partners to help us bring these new pacemakers to the commercial market.
The Nuclear Battery Company With a Vision
Ready to power your next innovation or learn more about our technology?
Contact Us Today





